In the vast majority of patients with low back pain, symptoms can be attributed to nonspecific mechanical factors. However, in a much smaller percentage of patients, the cause of back pain may be something more serious, such as cancer, cauda equina syndrome, spinal infection, spinal compression fractures, spinal stress fractures, ankylosing spondylitis, or aneurysm.
^ Jump up to: a b c d American College of Occupational and Environmental Medicine (February 2014), "Five Things Physicians and Patients Should Question", Choosing Wisely: an initiative of the ABIM Foundation, American College of Occupational and Environmental Medicine, archived from the original on 11 September 2014, retrieved 24 February 2014, which cites
John Wolf is Onnit's Chief Fitness Officer, and an expert in unconventional training methods such as kettlebell, steel club, and suspension training. With 15-plus years of experience in the fitness industry, he has worked with rehab clients and athletes of all levels. He moves like Spider Man and can deadlift more than 500 pounds any day of the week.
Really a great content. Let me tell you first about hip flexor it is the engine through which our body moves. They control balance, our ability to sit, stand, twist, reach, bend, walk and step. One of my patient also suffering from same problem but due to lack of money he was unable to afford a treatment. So i recommend him a program to unlock hip flexor. If anyone wants they can check it out here ;- https://tinyurl.com/y8yaqs2s Report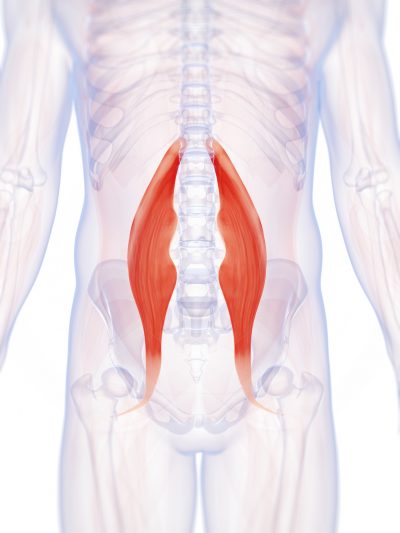
Vertebroplasty and kyphoplasty are minimally invasive treatments to repair compression fractures of the vertebrae caused by osteoporosis. Vertebroplasty uses three-dimensional imaging to assist in guiding a fine needle through the skin into the vertebral body, the largest part of the vertebrae. A glue-like bone cement is then injected into the vertebral body space, which quickly hardens to stabilize and strengthen the bone and provide pain relief. In kyphoplasty, prior to injecting the bone cement, a special balloon is inserted and gently inflated to restore height to the vertebral structure and reduce spinal deformity.

To ease the pain and lower your odds of an injury, don’t try to do too much at once. “Start with just 10 minutes,” says Arina Garg, MD, a rheumatology fellow at The Center for Excellence for Arthritis and Rheumatology at the Louisiana University Health Sciences Center. “Every few days, increase that time by 5 to 10 minutes.” Your goal is to work up to 30 minutes of aerobic exercise, 5 days a week.

Meanwhile, many non-dangerous problems can cause amazingly severe back pain. A muscle cramp is a good analogy — just think about how painful a Charley horse is! Regardless of what’s actually going on in there, muscle pain is probably the main thing that back pain patients are feeling. The phenomenon of trigger points — tiny muscle cramps, basically11 — could be the entire problem, or a complication that’s more painful and persistent than the original problem. It’s hard to overstate how painful trigger points can be, but they are not dangerous to anything but your comfort.
Just because your hip flexor region feels sore doesn’t necessarily mean the muscles there are tight — in fact, they might need strengthening. This is where that sports science debate we mentioned earlier comes into play. It’s important to identify whether you’re tight or if the muscles are weak. Again, the Thomas Test will help you identify if you’re maybe stretching something that actually needs strengthening.

Icing a joint that’s inflamed because of arthritis or bursitis can lower inflammation and help with hip pain. “If it’s very painful, I sometimes tell patients to ice four or five times daily for about 10 to 15 minutes,” says Amy Humphrey, DPT, a physical therapist at Body Dynamics, Inc. in Arlington, Va. Use an ice pack, wrap a towel around it, and put it where you feel the pain.

Im a skateboarder and a couple weeks ago i skated alot every day and my lefy hip was starting to get sore. But of course i couldnt resist skating so i kept skating and it got worse and worse to the point i couldnt really skate at all without my hip hurting but of course i would still mess around on the board doing tiny tricks but a couple days ago i was just skating around not really doing tricks and i slipped and kicked my leg out and REALLY hurt my hip and thought i tore a tendon or something and couldnt walk for two days, but its gotten alot better and i can walk fairly normal and i ice it everyday but whenever i stretch it its just a really sharp pain it doesnt feel like im stretching it. What do i do when all the stretch does is make a sharp pain? How do i strengthen my hip? And how long would it take to strengthen my hip to full strength again? Because i cant stand not being able to skate. Please reply so i can skate as soon as possible thank you

The lumbar (or lower back) region is made up of five vertebrae (L1–L5), sometimes including the sacrum. In between these vertebrae are fibrocartilaginous discs, which act as cushions, preventing the vertebrae from rubbing together while at the same time protecting the spinal cord. Nerves come from and go to the spinal cord through specific openings between the vertebrae, providing the skin with sensations and messages to muscles. Stability of the spine is provided by the ligaments and muscles of the back and abdomen. Small joints called facet joints limit and direct the motion of the spine.[30]
Meanwhile, many non-dangerous problems can cause amazingly severe back pain. A muscle cramp is a good analogy — just think about how painful a Charley horse is! Regardless of what’s actually going on in there, muscle pain is probably the main thing that back pain patients are feeling. The phenomenon of trigger points — tiny muscle cramps, basically11 — could be the entire problem, or a complication that’s more painful and persistent than the original problem. It’s hard to overstate how painful trigger points can be, but they are not dangerous to anything but your comfort.
Low back pain that lasts at least one day and limits activity is a common complaint.[7] Globally, about 40% of people have LBP at some point in their lives,[7] with estimates as high as 80% of people in the developed world.[22] Approximately 9 to 12% of people (632 million) have LBP at any given point in time, and nearly one quarter (23.2%) report having it at some point over any one-month period.[7][8] Difficulty most often begins between 20 and 40 years of age.[1] Low back pain is more common among people aged 40–80 years, with the overall number of individuals affected expected to increase as the population ages.[7]
Sleeping in an awkward position can cause you to be in pain from the moment you wake up. The best sleeping position for lower back pain may be sleeping on your side with your knees drawn up close to your chest (also known as the fetal position). Placing a pillow or two between your legs, while sleeping on your side, helps to reduce stress on your lower back. Sleeping on a too soft mattress can also cause lower back pain. A firmer mattress is best.
Arthritis: The spondyloarthropathies are inflammatory types of arthritis that can affect the lower back and sacroiliac joints. Examples of spondyloarthropathies include reactive arthritis (Reiter's disease), ankylosing spondylitis, psoriatic arthritis, and the arthritis of inflammatory bowel disease. Each of these diseases can lead to low back pain and stiffness, which is typically worse in the morning. These conditions usually begin in the second and third decades of life. They are treated with medications directed toward decreasing the inflammation. Newer biologic medications have been greatly successful in both quieting the disease and stopping its progression.

Fitness level: Back pain is more common among people who are not physically fit. Weak back and abdominal muscles may not properly support the spine. “Weekend warriors”—people who go out and exercise a lot after being inactive all week—are more likely to suffer painful back injuries than people who make moderate physical activity a daily habit. Studies show that low-impact aerobic exercise is beneficial for the maintaining the integrity of intervertebral discs.
Apply the above concept to your hips. When you sit, your hips are in a "flexed" position. Therefore, the muscles that flex your hips are in a shortened state. You probably spend at least a third of your day sitting down. Think about how much time those hip flexor muscles stay shortened. A lot. Over time, they become tighter and tighter until you look like the old man in the picture. So unless you want to look like that, perform the stretches shown below.
Lay on your back on your mat and pull your knees to your chest. Place your hands on the inside arches of your feet and open your knees wider than shoulder-width apart. Keeping your back pressed into the mat as much as possible, press your feet into hands while pulling down on feet, creating resistance. Breathe deeply and hold for at least 30 seconds.
Spinal fusion is used to strengthen the spine and prevent painful movements in people with degenerative disc disease or spondylolisthesis (following laminectomy). The spinal disc between two or more vertebrae is removed and the adjacent vertebrae are “fused” by bone grafts and/or metal devices secured by screws. The fusion can be performed through the abdomen, a procedure known as an anterior lumbar interbody fusion, or through the back, called posterior fusion. Spinal fusion may result in some loss of flexibility in the spine and requires a long recovery period to allow the bone grafts to grow and fuse the vertebrae together. Spinal fusion has been associated with an acceleration of disc degeneration at adjacent levels of the spine.
myDr myDr provides comprehensive Australian health and medical information, images and tools covering symptoms, diseases, tests, medicines and treatments, and nutrition and fitness.Related ArticlesSciatica: symptoms, causes and diagnosisSciatica is characterised by pain deep in the buttock often radiating down the back of the leg. One Sciatica: treatmentMost sciatica gets better within a few weeks. If not, there are treatments that may help relieve youNeck pain: symptoms and causesKnowing the symptoms of your neck pain and when to see a doctor can help in finding the cause and geNeck pain: treatmentTreatment for neck pain depends on the cause and how severe it is. Neck pain treatment, includiOffice ergonomics: workstation comfort and safetyComputer users often develop aches and pains. Avoid discomfort by setting up your workstation accordPilates no better for low back painCochrane researchers found no significant difference between Pilates and other exercises for pain anDormant butt syndrome is linked to knee and back painDormant butt syndrome, characterised by weak glute muscles and tight hip flexors, can be caused by sSpinal surgery for low back pain over-optimisticSpinal fusion surgery has at best a 50% success rate for the initial operation and patients would beVideo: Reframing pain to overcome lower back painReliance on opioid painkillers and unnecessary back surgeries may be preventing us from beating loweAdvertisement
Just because your hip flexor region feels sore doesn’t necessarily mean the muscles there are tight — in fact, they might need strengthening. This is where that sports science debate we mentioned earlier comes into play. It’s important to identify whether you’re tight or if the muscles are weak. Again, the Thomas Test will help you identify if you’re maybe stretching something that actually needs strengthening.
Pregnancy symptoms can vary from woman to woman, and not all women experience the same symptoms. When women do experience pregnancy symptoms they may include symptoms include missed menstrual period, mood changes, headaches, lower back pain, fatigue, nausea, breast tenderness, and heartburn. Signs and symptoms in late pregnancy include leg swelling and shortness of breath. Options for relief of pregnancy symptoms include exercise, diet, and other lifestyle changes.
Initial management with non–medication based treatments is recommended.[6] NSAIDs are recommended if these are not sufficiently effective.[6] Normal activity should be continued as much as the pain allows.[2] Medications are recommended for the duration that they are helpful.[13] A number of other options are available for those who do not improve with usual treatment. Opioids may be useful if simple pain medications are not enough, but they are not generally recommended due to side effects.[4][13] Surgery may be beneficial for those with disc-related chronic pain and disability or spinal stenosis.[14][15] No clear benefit has been found for other cases of non-specific low back pain.[14] Low back pain often affects mood, which may be improved by counseling or antidepressants.[13][16] Additionally, there are many alternative medicine therapies, including the Alexander technique and herbal remedies, but there is not enough evidence to recommend them confidently.[17] The evidence for chiropractic care[18] and spinal manipulation is mixed.[17][19][20][21]

Lay on your back on your mat and pull your knees to your chest. Place your hands on the inside arches of your feet and open your knees wider than shoulder-width apart. Keeping your back pressed into the mat as much as possible, press your feet into hands while pulling down on feet, creating resistance. Breathe deeply and hold for at least 30 seconds.

Stop listening to other people’s horror stories. You know the scenario: You are bent over in obvious pain, waiting to see the doctor, and the person next to you tells you a 10-minute tale of how their Uncle Gordon had low back pain that required injections and surgery. But the pain still didn’t go away. Stop listening to these terrible stories. Most low back pain is short-lived and can be managed quite effectively with exercise and postural correction. Of course, some low back conditions are serious and require surgery, but that is a conversation you should have with your doctor, not the guy in the waiting room.

The treatment of lumbar strain consists of resting the back (to avoid reinjury), medications to relieve pain and muscle spasm, local heat applications, massage, and eventual (after the acute episode resolves) reconditioning exercises to strengthen the low back and abdominal muscles. Initial treatment at home might include heat application, acetaminophen (Tylenol) or ibuprofen (Advil, Motrin), and avoiding reinjury and heavy lifting. Prescription medications that are sometimes used for acute low back pain include anti-inflammatory medications, such as sulindac (Clinoril), naproxen (Naprosyn), and ketorolac (Toradol) by injection or by mouth, muscle relaxants, such as carisoprodol (Soma), cyclobenzaprine (Flexeril), methocarbamol (Robaxin), and metaxalone (Skelaxin), as well as analgesics, such as tramadol (Ultram).

Bone scans are used to detect and monitor infection, fracture, or disorders in the bone. A small amount of radioactive material is injected into the bloodstream and will collect in the bones, particularly in areas with some abnormality. Scanner-generated images can be used to identify specific areas of irregular bone metabolism or abnormal blood flow, as well as to measure levels of joint disease.

While a sharp pain in the hip, groin, pelvis, or thigh is an obvious sign of a hip flexor injury, pain in the lower back and leg are easy to misdiagnose. After all, it’s natural to assume that radiating pain in the leg or lower back originate from these areas. Unfortunately, diagnosing the source of a patient’s pain is not always straightforward. In fact, it’s possible for patients to go years with a misdiagnosed injury.
Take a step back and think about where you spend most of your day. If you're a young athlete, you probably spend most of your time at school or maybe work or practice and even a little time at home, if you're lucky. Now think about what position your body is in during those periods. I would bet that you spend most of your day sitting down. You may walk to class or run in practice, but the majority of your day is spent in a seated position. 
Stop searching for a miracle cure for your back pain. We’ve all seen the advertisements that promise a miracle cure for your low back pain. Hanging by your feet on an inversion table, rubbing healing balms on your back or spending money on fancy computerized traction devices all sound effective but the evidence indicates that many of these miracle cures are not beneficial.
The outlook for low back pain absolutely depends on its precise cause. For example, acute strain injuries generally heal entirely with minimal treatment. On the other hand, bony abnormalities that are irritating the spinal cord can require significant surgical repair and the outlook depends on the surgical result. Long-term optimal results often involve exercise rehabilitation programs that can involve physical therapists.
The big idea of classification-based cognitive functional therapy (CB-CFT or just CFT) is that most back pain has nothing to do with scary spinal problems and so the cycle of pain and disability can be broken by easing patient fears and anxieties. For this study, CFT was tried with 62 patients and compared to 59 who were treated with manual therapy and exercise. The CFT group did better: a 13-point boost on a 100-point disability scale, and 3 points on a 10-point pain scale. As the authors put it for BodyInMind.org, “Disabling back pain can change for the better with a different narrative and coping strategies.” These results aren’t proof that the confidence cure works, but they are promising.
Hamstring squeeze. Use the machine that works your hamstrings; you will either lie on your stomach or sit with a pad behind your knee. Push against the pad, moving your knee up toward the ceiling or backward (depending on which position you’re in). “In other words, bend your knees,” Pariser says. But to avoid cramps in your hamstring muscles, don’t bend your knee so much that your heels are too close to your buttocks.
There is a significant overlap of nerve supply to many of the discs, muscles, ligaments, and other spinal structures, and it can be difficult for the brain to accurately sense which is the cause of the pain. For example, a degenerated or torn lumbar disc can feel the same as a pulled muscle – both creating inflammation and painful muscle spasm in the same area. Muscles and ligaments heal rapidly, while a torn disc may or may not. The time course of pain helps determine the cause.

It is unclear if among those with non-chronic back pain alternative treatments are useful.[84] For chiropractic care or spinal manipulation therapy (SMT) it is unclear if it improves outcomes more or less than other treatments.[18] Some reviews find that SMT results in equal or better improvements in pain and function when compared with other commonly used interventions for short, intermediate, and long-term follow-up;[19][20][85] other reviews find it to be no more effective in reducing pain than either inert interventions, sham manipulation, or other treatments, and conclude that adding SMT to other treatments does improve outcomes.[17][21] National guidelines reach different conclusions, with some not recommending spinal manipulation, some describing manipulation as optional, and others recommending a short course for those who do not improve with other treatments.[3] A 2017 review recommended spinal manipulation based on low quality evidence.[6] Manipulation under anaesthesia, or medically assisted manipulation, has not enough evidence to make any confident recommendation.[86]
How to: Position yourself on your hands and knees, in tabletop position. Engage your abs engaged by pulling your belly button in towards your spine (a). Keeping your hips pointed towards the ground and leg bent to a 90-degree angle, raise your left knee out to the side as high as you can (b). Pause at the top, then return to starting position (c). Repeat, then switch legs.

Deanna is an ACE® certified personal trainer, Balanced Body® Pilates instructor, and NASM® Fitness Nutrition Specialist. She is passionate about inspiring others to lead a healthier lifestyle through fun workouts and healthy food. When she’s not creating new workouts and recipes for her blog The Live Fit Girls she enjoys running with her two dogs and traveling.

Iliopsoas syndrome, which is also called psoas syndrome or iliopsoas tendonitis, occurs when the iliopsoas muscles are injured. Lower back pain is the most common symptom; however, pain can also occur in the hip, thigh, or leg. The iliopsoas bursa, which is a fluid-filled sac located on the inside of the hip that reduces rubbing and friction, is also likely to become inflamed due to the proximity of the two structures. When this happens, the inflamed bursae will make it difficult to move.
In both younger and older patients, vertebral fractures take weeks to heal with rest and pain relievers. Compression fractures of vertebrae associated with osteoporosis can also be treated with a procedure called vertebroplasty or kyphoplasty, which can help to reduce pain. In this procedure, a balloon is inflated in the compressed vertebra, often returning some of its lost height. Subsequently, a "cement" (methymethacrylate) is injected into the balloon and remains to retain the structure and height of the body of the vertebra. Pain is relieved as the height of the collapsed vertebra is restored.

Health Tools Baby Due Date CalculatorBasal Metabolic Rate CalculatorBody Mass Index (BMI) CalculatorCalories Burned CalculatorChild Energy Requirements CalculatorDaily Calcium Requirements CalculatorDaily Fibre Requirements CalculatorIdeal Weight CalculatorInfectious Diseases Exclusion Periods ToolOvulation CalculatorSmoking Cost CalculatorTarget Heart Rate CalculatorWaist-to-hip Ratio Calculator Risk Tests Depression Self-AssessmentErectile Dysfunction ToolMacular Degeneration ToolOsteoporosis Risk TestProstate Symptoms Self-Assessment
The site navigation utilizes arrow, enter, escape, and space bar key commands. Left and right arrows move across top level links and expand / close menus in sub levels. Up and Down arrows will open main level menus and toggle through sub tier links. Enter and space open menus and escape closes them as well. Tab will move on to the next part of the site rather than go through menu items.
When a muscle contracts, it shortens. Take the biceps for example. Without getting too technical, the biceps are attached at the forearm and shoulder. When your biceps contract, they shorten and bring those two points closer together. When you rest, the muscle returns to its normal length, and the two points move farther away. Constantly contracting your biceps over a long period of time would cause them to get shorter, even at rest.
Many athletes-from the weekend warrior to the elite professional athlete-buck up their strength, pop some over-the-counter pain medication, and tolerate the pain for the sake of the game and personal enjoyment. But avoiding medical help can lead to further and more serious injury. Without medical help, the anatomic damage can sometimes lead to permanent exclusion from sporting activities.
Recovering from a hip flexor injury can take time, but proper supervision and guidance from a musculoskeletal professional can minimize downtime and pain. Additionally, there are a few stretches you can do at home to recover from a hip flexor injury. The following stretch increases hip flexor dexterity, while helping alleviate pain in and around the hip and upper thigh.
There are a number of ways to classify low back pain with no consensus that any one method is best.[5] There are three general types of low back pain by cause: mechanical back pain (including nonspecific musculoskeletal strains, herniated discs, compressed nerve roots, degenerative discs or joint disease, and broken vertebra), non-mechanical back pain (tumors, inflammatory conditions such as spondyloarthritis, and infections), and referred pain from internal organs (gallbladder disease, kidney stones, kidney infections, and aortic aneurysm, among others).[5] Mechanical or musculoskeletal problems underlie most cases (around 90% or more),[5][34] and of those, most (around 75%) do not have a specific cause identified, but are thought to be due to muscle strain or injury to ligaments.[5][34] Rarely, complaints of low back pain result from systemic or psychological problems, such as fibromyalgia and somatoform disorders.[34]
Intervertebral disc degeneration is one of the most common mechanical causes of low back pain, and it occurs when the usually rubbery discs lose integrity as a normal process of aging. In a healthy back, intervertebral discs provide height and allow bending, flexion, and torsion of the lower back. As the discs deteriorate, they lose their cushioning ability.

But moving is important for hip and knee OA. It causes your joints to compress and release, bringing blood flow, nutrients, and oxygen into the cartilage. “This can help prolong the function and longevity of your joints,” says Eric Robertson, DPT, a physical therapist and associate professor of clinical physical therapy at the University of Southern California.

There is controversy and scientific uncertainty about trigger points. It’s undeniable that mammals suffer from sensitive spots in our soft tissues … but their nature remains unclear, and the “tiny cramp” theory could be wrong. The tiny cramp theory is formally known as the “expanded integrated hypothesis,” and it has been prominently criticized by Quintner et al (and not many others). However, it’s the mostly widely accepted explanation for now. BACK TO TEXT

The treatment of lumbar strain consists of resting the back (to avoid reinjury), medications to relieve pain and muscle spasm, local heat applications, massage, and eventual (after the acute episode resolves) reconditioning exercises to strengthen the low back and abdominal muscles. Initial treatment at home might include heat application, acetaminophen (Tylenol) or ibuprofen (Advil, Motrin), and avoiding reinjury and heavy lifting. Prescription medications that are sometimes used for acute low back pain include anti-inflammatory medications, such as sulindac (Clinoril), naproxen (Naprosyn), and ketorolac (Toradol) by injection or by mouth, muscle relaxants, such as carisoprodol (Soma), cyclobenzaprine (Flexeril), methocarbamol (Robaxin), and metaxalone (Skelaxin), as well as analgesics, such as tramadol (Ultram).
Recurring back pain resulting from improper body mechanics is often preventable by avoiding movements that jolt or strain the back, maintaining correct posture, and lifting objects properly. Many work-related injuries are caused or aggravated by stressors such as heavy lifting, contact stress (repeated or constant contact between soft body tissue and a hard or sharp object), vibration, repetitive motion, and awkward posture. Using ergonomically designed furniture and equipment to protect the body from injury at home and in the workplace may reduce the risk of back injury.

As with any sort of pain, it's crucial to figure out the source so you can properly treat it. Sharp or stabbing pain that extends beyond your low back or is accompanied by symptoms like abdominal pain, nausea, and vomiting, could be signs of various other conditions and definitely warrant a trip to the doctor. If you have a history of lower back injuries or disc problems, always see your doctor before trying any new exercise.
True numbness is not just a dead/heavy feeling (which is common, and caused even by minor muscular dysfunction in the area), but a significant or complete lack of sensitivity to touch. You have true numbness when you have patches of skin where you cannot feel light touch. Such areas might still be sensitive to pressure: you could feel a poke, but as if it was through a layer of rubber. Most people have experienced true numbness at the dentist. BACK TO TEXT
AAOS does not endorse any treatments, procedures, products, or physicians referenced herein. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific orthopaedic advice or assistance should consult his or her orthopaedic surgeon, or locate one in your area through the AAOS Find an Orthopaedist program on this website.
2016 — More editing, more! Added some better information about pain being a poor indicator, and the role of myofascial trigger points. This article has become extremely busy in the last couple months — about 4,000 readers per day, as described here — so I am really polishing it and making sure that it’s the best possible answer to people’s fears about back pain.

If your hips are killing you, you probably spend a lot of time sitting – in the car, at work, on that spinning seat – which puts your hips in near-constant “flexion”, says Cori Lefkowith, NASM-certified personal trainer and owner of Redefining Strength in Orange County, California. Even running involves a repetitive flexion movement that can cause pain.
In terms of diagnosing hip pain, typically a patient will expect when they come in to be asked about their symptoms, and it’s very important to find out when did these symptoms start, how long they have been going on, how frequent they are, if they come on in the morning or the evening, do they come on with any certain activity, and if there is something that makes it better or worse. The intensity of the pain is also important. Does it have any associated radiating symptoms? Is it localized in one spot or does it move? After getting a history and finding out what type of pain the patient is having, which also includes whether the pain is dull, aching, sharp, or intense, then it’s important to do a good physical exam. The physical examination involves testing the muscle strength, testing for sensation, doing provocative maneuvers which might help us rule out one type of injury from another.

4. Just swing it. For the front-to-back hip swing stretch, lie on the left side with hips stacked, propped up on the left elbow. Bend the left leg to a 90-degree angle and raise the right leg to hip level with toes pointed. Keep abs tight and swing the right leg all the way in front, then swing it all the way to the back, squeezing the booty along the way. Switch sides.
Start kneeling on your mat with knees hip-width apart and hips directly over knees. Press your shins and the tops of your feet into the mat. Bring your hands to your low back, fingers pointing down, and rest palms above glutes. Inhale and lift your chest, and then slowly start to lean your torso back. From here, bring your right hand to rest on your right heel and then your left hand to your left heel. (If you can't reach your heels, turn your toes under; it will be easier to reach your heels in this modification.) Press your thighs forward so they are perpendicular to the floor. Keep your head in a relatively neutral position or, if it doesn't strain your neck, drop it back. Hold for 30 seconds. To come out of the pose, bring your hands to your hips and slowly, leading with your chest, lift your torso as you press the thighs down toward the floor.

