Avascular necrosis (also called osteonecrosis). This condition happens when blood flow to the hip bone slows and the bone tissue dies. Although it can affect other bones, avascular necrosis most often happens in the hip. It can be caused by a hip fracture or dislocation, or from the long-term use of high-dose steroids (such as prednisone), among other causes.
It is unclear if among those with non-chronic back pain alternative treatments are useful.[84] For chiropractic care or spinal manipulation therapy (SMT) it is unclear if it improves outcomes more or less than other treatments.[18] Some reviews find that SMT results in equal or better improvements in pain and function when compared with other commonly used interventions for short, intermediate, and long-term follow-up;[19][20][85] other reviews find it to be no more effective in reducing pain than either inert interventions, sham manipulation, or other treatments, and conclude that adding SMT to other treatments does improve outcomes.[17][21] National guidelines reach different conclusions, with some not recommending spinal manipulation, some describing manipulation as optional, and others recommending a short course for those who do not improve with other treatments.[3] A 2017 review recommended spinal manipulation based on low quality evidence.[6] Manipulation under anaesthesia, or medically assisted manipulation, has not enough evidence to make any confident recommendation.[86]
Discography may be used when other diagnostic procedures fail to identify the cause of pain. This procedure involves the injection of a contrast dye into a spinal disc thought to be causing low back pain. The fluid’s pressure in the disc will reproduce the person’s symptoms if the disc is the cause. The dye helps to show the damaged areas on CT scans taken following the injection. Discography may provide useful information in cases where people are considering lumbar surgery or when their pain has not responded to conventional treatments.


When we stand, the lower back is functioning to support the weight of the upper body. When we bend, extend, or rotate at the waist, the lower back is involved in the movement. Therefore, injury to the structures important for weight bearing, such as the bony spine, muscles, tendons, and ligaments, often can be detected when the body is standing erect or used in various movements.
Two types of strength-training moves that may benefit the lower back are flexion and extension exercises. In flexion exercises, you bend forward to stretch the muscles of the back and hips. In extension exercises, you bend backward to develop the muscles that support the spine. One example is doing leg lifts while lying on your stomach. Depending on the cause of your back pain, there are some exercises you should not do. If you have back pain, make sure to talk to your doctor about what exercises are safe for you.
The treatment of lumbar strain consists of resting the back (to avoid reinjury), medications to relieve pain and muscle spasm, local heat applications, massage, and eventual (after the acute episode resolves) reconditioning exercises to strengthen the low back and abdominal muscles. Initial treatment at home might include heat application, acetaminophen (Tylenol) or ibuprofen (Advil, Motrin), and avoiding reinjury and heavy lifting. Prescription medications that are sometimes used for acute low back pain include anti-inflammatory medications, such as sulindac (Clinoril), naproxen (Naprosyn), and ketorolac (Toradol) by injection or by mouth, muscle relaxants, such as carisoprodol (Soma), cyclobenzaprine (Flexeril), methocarbamol (Robaxin), and metaxalone (Skelaxin), as well as analgesics, such as tramadol (Ultram).
Your hip labrum is a band of cartilage-like tissue that courses around the outer rim of your hip socket. This labrum helps to support the joint and deepen the socket. Sometimes overuse or an injury to your hip can cause a tear in your labrum. A hip labrum tear may result in a condition called femoroacetabular impingement (FAI). When this happens, hip pain may result, and exercises to stretch and stabilize your hip may be performed.
If most inner-thigh openers feel too easy (and your ankles and knees are injury-free), try Frog Pose. Get down on all fours, with palms on the floor and your knees on blankets or a mat (roll your mat lengthwise, like a tortilla, and place it under your knees for more comfort). Slowly widen your knees until you feel a comfortable stretch in your inner thighs, keeping the inside of each calf and foot in contact with the floor. Make sure to keep your ankles in line with your knees. Lower down to your forearms. Stay here for at least 30 seconds.
Strength training is another key part of the “do” category, Dr. Vasileff says. “It’s a good idea to focus on quad, hamstring, and glute strength,” he says. These muscles surround your hips and provide support, along with your core—which is another area to focus on. “Strengthening your core helps to normalize your walking pattern and stabilize how your pelvis and hips move,” Dr. Vasileff says. That translates to less pain and better hip mobility.
This Australian study concluded that “prognosis is moderately optimistic for patients with chronic low back pain,” contradicting the common fear that any low back pain that lasts longer than 6-9 weeks will become a long-term chronic problem. This evidence is the first of its kind, a rarity in low back pain research, a field where almost everything has been studied to death. “Many studies provide good evidence for the prognosis of acute low back pain,” the authors explain. “Relatively few provide good evidence for the prognosis of chronic low back pain.”
This standard recommendation reinforces the alarming idea that low back pain that lasts longer than a few weeks is Really Bad News. It’s not. It’s a clue. It’s a reason for concern and alertness. But many cases of low back pain that last for 6 weeks will still go away. Once again, see the 2009 research published in the British Medical Journal, which showed that more than 30% of patients with “new” chronic low back pain will still recover without treatment. BACK TO TEXT
We implement a variety of security measures to maintain the safety of your personal information when you place an order or enter, submit, or access any information on our website. We incorporate physical, electronic, and administrative procedures to safeguard the confidentiality of your personal information, including Secure Sockets Layer (SSL) for the encryption of all financial transactions through the website. We use industry-standard, 256bit SSL encryption to protect your personal information online, and we also take several steps to protect your personal information in our facilities. For example, when you visit the website, you access servers that are kept in a secure physical environment, behind a locked cage and a hardware firewall. After a transaction, your credit card information is not stored on our servers. 
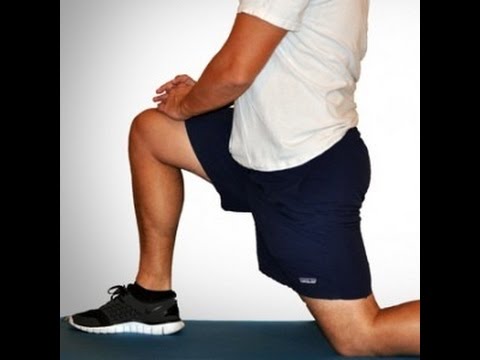
Avoiding injury to the low back is a method of preventing low back pain. Additionally, conditioning exercise programs designed to strengthen the lumbar area and adjacent tissues can help to minimize risk of injury to the low back. Specific programs to relieve and prevent back pain can be designed with the help of physical therapists and other treating health-care professionals.
The hip flexors play an important role in everyday mobility and exercise. Involved in pulling the knee toward the hip, most movements either directly or indirectly use the hip flexors. That’s why even the slightest injury can cause great discomfort. Learn how you can recover from a hip flexor injury, and what precautions can be taken to avoid them.
People understandably assume that the worst back pain is the scariest. In fact, pain intensity is a poor indicator of back pain ominousness,10 and some of the worst causes are actually the least painful (especially in the early stages). For instance, someone could experience the symptoms of cauda equinae syndrome, and be in real danger of a serious and permanent injury to their spine, but have surprisingly little pain — even none at all in some cases!
Lie on your back with your knees bent and your feet flat on the floor. Tighten the muscles in your buttocks, then lift your hips off the ground and hold for about five seconds before slowly lowering yourself back down. Be sure to breathe throughout the exercise. As with the first exercise, you can work up to doing 30 repetitions, resting for a few seconds (or longer) between each. “If you start to get tired, stop and rest for a couple of minutes,” Pariser says.

The hip flexors play an important role in everyday mobility and exercise. Involved in pulling the knee toward the hip, most movements either directly or indirectly use the hip flexors. That’s why even the slightest injury can cause great discomfort. Learn how you can recover from a hip flexor injury, and what precautions can be taken to avoid them.


