The good news is that there are plenty of good hip stretches out there that you can do to relieve discomfort, decrease tightness, and increase mobility in your hips. Since your hips are involved in so many of the movements you make (both inside and outside of the gym) stretching them is a great way to keep them feeling good and ready to work for you. Add some of the 12 hip stretches Atkins demos below to the end of your workout, or spend 10 minutes each day just doing a few of them, to improve mobility in your hips.
3. Tendinitis and bursitis Many tendons around the hip connect the muscles to the joint. These tendons can easily become inflamed if you overuse them or participate in strenuous activities. One of the most common causes of tendinitis at the hip joint, especially in runners, is iliotibial band syndrome — the iliotibial band is the thick span of tissue that runs from the outer rim of your pelvis to the outside of your knee.
Health care professionals diagnose hip pain with a history and physical examination. Physical examination maneuvers, such as internally and externally rotating the hip, can be used to detect pain-aggravating positions. Tenderness can be elicited by palpating over inflamed areas. Straight leg raising can detect signs of sciatica. A health care professional may use imaging studies, including X-rays, CT scans, and MRI scans, to further define the causes of hip pain. Sometimes, nuclear medicine bone scans are used to image inflamed or fractured bone.
Two types of strength-training moves that may benefit the lower back are flexion and extension exercises. In flexion exercises, you bend forward to stretch the muscles of the back and hips. In extension exercises, you bend backward to develop the muscles that support the spine. One example is doing leg lifts while lying on your stomach. Depending on the cause of your back pain, there are some exercises you should not do. If you have back pain, make sure to talk to your doctor about what exercises are safe for you.
Why is back pain still a huge problem? Maybe this: “It is extremely difficult to alter the potentially disabling belief among the lay public that low back pain has a structural mechanical cause. An important reason for this is that this belief continues to be regularly reinforced by the conditions of care of a range of ‘hands-on’ providers, for whom idiosyncratic variations of that view are fundamental to their professional existence.”
2016 — More editing, more! Added some better information about pain being a poor indicator, and the role of myofascial trigger points. This article has become extremely busy in the last couple months — about 4,000 readers per day, as described here — so I am really polishing it and making sure that it’s the best possible answer to people’s fears about back pain.
Health Tools Baby Due Date CalculatorBasal Metabolic Rate CalculatorBody Mass Index (BMI) CalculatorCalories Burned CalculatorChild Energy Requirements CalculatorDaily Calcium Requirements CalculatorDaily Fibre Requirements CalculatorIdeal Weight CalculatorInfectious Diseases Exclusion Periods ToolOvulation CalculatorSmoking Cost CalculatorTarget Heart Rate CalculatorWaist-to-hip Ratio Calculator Risk Tests Depression Self-AssessmentErectile Dysfunction ToolMacular Degeneration ToolOsteoporosis Risk TestProstate Symptoms Self-Assessment
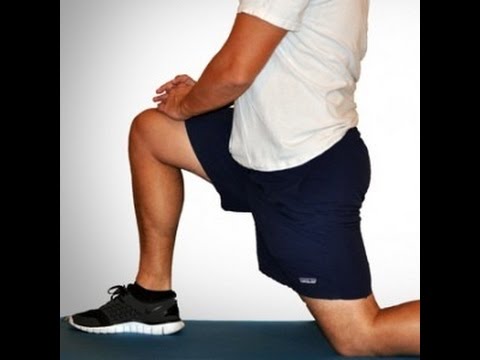
Since the hip flexors are so easy to overuse and strain, it is important to stretch them before exercise or strenuous activity. Because of their connectedness to other muscle groups in the legs (like the quadriceps), it is important to stretch the muscle group as a whole, not individually. This ensures that the entire area is warmed up and ready for the strain of exercise or activity, not just one or two individual muscles.
Endometriosis (when the uterus lining grows somewhere else) can cause pelvic tenderness, which some women describe as hip pain. Pain from the back and spine also can be felt around the buttocks and hip, Siegrist says. Sciatica, a pinched nerve, typically affects one side of the body and can cause pain in the back of the right or left hip — the pain from sciatica can start in your lower back and travel down to your buttocks and legs.

Athletes are at greater risk of sustaining a lumber spine injury due to physical activity. Whether the sport is skiing, basketball, football, gymnastics, soccer, running, golf, or tennis-the spine undergoes a lot of stress, absorption of pressure, twisting, turning, and even bodily impact. This strenuous activity puts stress on the back that can cause injury to even the finest and most fit athletes.

Discography may be used when other diagnostic procedures fail to identify the cause of pain. This procedure involves the injection of a contrast dye into a spinal disc thought to be causing low back pain. The fluid’s pressure in the disc will reproduce the person’s symptoms if the disc is the cause. The dye helps to show the damaged areas on CT scans taken following the injection. Discography may provide useful information in cases where people are considering lumbar surgery or when their pain has not responded to conventional treatments.

Health Tools Baby Due Date CalculatorBasal Metabolic Rate CalculatorBody Mass Index (BMI) CalculatorCalories Burned CalculatorChild Energy Requirements CalculatorDaily Calcium Requirements CalculatorDaily Fibre Requirements CalculatorIdeal Weight CalculatorInfectious Diseases Exclusion Periods ToolOvulation CalculatorSmoking Cost CalculatorTarget Heart Rate CalculatorWaist-to-hip Ratio Calculator Risk Tests Depression Self-AssessmentErectile Dysfunction ToolMacular Degeneration ToolOsteoporosis Risk TestProstate Symptoms Self-Assessment
Lie on your back with your knees bent and your feet flat on the floor. Tighten the muscles in your buttocks, then lift your hips off the ground and hold for about five seconds before slowly lowering yourself back down. Be sure to breathe throughout the exercise. As with the first exercise, you can work up to doing 30 repetitions, resting for a few seconds (or longer) between each. “If you start to get tired, stop and rest for a couple of minutes,” Pariser says.
In order to validate your account, please either send an email from your .mil email address or send in a snapshot of your military ID to our customer service help desk. Blacking out rank and or post is acceptable. In either case, please include the civilian email address or whichever email address you have registered with Onnit.com somewhere in the message body so we know which account to verify. Please setup an account with Onnit.com prior to submitting your request.
Nonsteroidal anti-inflammatory drugs (NSAIDS) relieve pain and inflammation and include OTC formulations (ibuprofen, ketoprofen, and naproxen sodium). Several others, including a type of NSAID called COX-2 inhibitors, are available only by prescription. Long-term use of NSAIDs has been associated with stomach irritation, ulcers, heartburn, diarrhea, fluid retention, and in rare cases, kidney dysfunction and cardiovascular disease. The longer a person uses NSAIDs the more likely they are to develop side effects. Many other drugs cannot be taken at the same time a person is treated with NSAIDs because they alter the way the body processes or eliminates other medications.
Compressive pain is a result of pressure or irritation on the spinal cord, nerves that leave the spine. For example, if an intervertebral disc herniates (usually called a ruptured disc) and pushes into the spinal canal, it can cause problems with the nerve. Usually this pressure or irritation causes pain, numbness, and muscle weakness where the nerve travels.
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed physician should be consulted for diagnosis and treatment of any and all medical conditions. Call 911 for all medical emergencies. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. Copyright 1997-2019, A.D.A.M., Inc. Duplication for commercial use must be authorized in writing by ADAM Health Solutions.
Physician specialties that evaluate and treat low back pain range from generalists to subspecialists.These specialties include emergency medicine physicians, general medicine, family medicine, internal medicine, gynecology, spine surgeons (orthopaedics and neurosurgery), rheumatology, pain management, and physiatry. Other health care providers for low back pain include physical therapists, chiropractors, massage therapists, psychologists, and acupuncturists.

Stop focusing on a specific diagnosis. Up to 85% of low back pain can be classified as "non-specific." This means that the origin of your pain cannot be localized to one specific structure or problem. While common diagnostic tests for low back pain can show the bones, discs, and joints with great detail, no test can tell the exact cause of your pain with 100% accuracy.
As with any sort of pain, it's crucial to figure out the source so you can properly treat it. Sharp or stabbing pain that extends beyond your low back or is accompanied by symptoms like abdominal pain, nausea, and vomiting, could be signs of various other conditions and definitely warrant a trip to the doctor. If you have a history of lower back injuries or disc problems, always see your doctor before trying any new exercise.
Disk tear. Small tears to the outer part of the disk (annulus) sometimes occur with aging. Some people with disk tears have no pain at all. Others can have pain that lasts for weeks, months, or even longer. A small number of people may develop constant pain that lasts for years and is quite disabling. Why some people have pain and others do not is not well understood.
If you develop a sudden onset of low back pain, a visit to your physical therapist can help you determine the correct things to do to manage your acute pain. Your physical therapist should be able to analyze your lifestyle, movements, and overall medical history to help determine the likely cause of your pain. By focusing on these mechanical causes of back pain, you can make a change that may give you relief.
Try Atrogel: Atrogel is amazing when it comes to soothing and easing pain, helping to relieve muscle aches, stiffness and bruising. It’s prepared using extracts of fresh arnica flowers and can be applied up to 4 times a day! Suitable for pregnant women and children, simply apply this lovely non-greasy formula to the affected area for some much-needed relief!
When was the last time you got on your gym's abductor or adductor machine and got in a good workout? It's probably been a while. Both are machines that don't get a lot of use, and they are often the target of coaches' ridicule on those "useless gym moves we should all skip" lists. Perhaps rightly so, especially if you're hopping on those machines hoping for a slimming effect.
Cycling: The repetitive movements of cycling can place a strain on your hip joints, not to mention that it can also affect your posture! If you really must cycle, make sure your bike is professionally fitted and that you properly warm up and stretch your hip flexors before getting on your bike. I’d recommend choosing an alternative though, or at least speaking to your doctor first!
Activity: Bed rest should be limited. Individuals should begin stretching exercises and resume normal daily activities as soon as possible, while avoiding movements that aggravate pain. Strong evidence shows that persons who continue their activities without bed rest following onset of low back pain appeared to have better back flexibility than those who rested in bed for a week. Other studies suggest that bed rest alone may make back pain worse and can lead to secondary complications such as depression, decreased muscle tone, and blood clots in the legs.
The management of low back pain often includes medications for the duration that they are beneficial. With the first episode of low back pain the hope is a complete cure; however, if the problem becomes chronic, the goals may change to pain management and the recovery of as much function as possible. As pain medications are only somewhat effective, expectations regarding their benefit may differ from reality, and this can lead to decreased satisfaction.[13]
Management of low back pain depends on which of the three general categories is the cause: mechanical problems, non-mechanical problems, or referred pain.[52] For acute pain that is causing only mild to moderate problems, the goals are to restore normal function, return the individual to work, and minimize pain. The condition is normally not serious, resolves without much being done, and recovery is helped by attempting to return to normal activities as soon as possible within the limits of pain.[3] Providing individuals with coping skills through reassurance of these facts is useful in speeding recovery.[1] For those with sub-chronic or chronic low back pain, multidisciplinary treatment programs may help.[53] Initial management with non–medication based treatments is recommended, with NSAIDs used if these are not sufficiently effective.[6]
"As compared to a conventional deadlift, the sumo allows for greater recruitment of the adductors and a more stabilizing emphasis for the abductors," says Lindsey Cormack, a competitive powerlifter and CrossFit trainer. "Training sumo may feel less stable at first, but the balance requirement is what allows you to effectively train both the abductors and adductors."
Before recommending exercises, physical therapists evaluate their patients to develop a routine that’s appropriate for their specific condition. Pariser says the following exercises, done at home and at the gym, are generally safe for everyone. “If a patient has already received a total hip replacement, however, certain precautions should be taken,” he says.
In addition to strengthening the core muscles, it's also important to address any mobility problems, says Jacque Crockford, M.S., C.S.C.S., exercise physiology content manager at American Council on Exercise, which can sometimes be what's causing pain. If specific movements like twisting or bending or extending your spine feel uncomfortable, there may be mobility (flexibility) issues at play. Doing some gentle stretching (like these yoga poses) might help. (If it gets worse with those stretches, stop and see a doctor.)

The multifidus muscles run up and down along the back of the spine, and are important for keeping the spine straight and stable during many common movements such as sitting, walking and lifting.[12] A problem with these muscles is often found in someone with chronic low back pain, because the back pain causes the person to use the back muscles improperly in trying to avoid the pain.[31] The problem with the multifidus muscles continues even after the pain goes away, and is probably an important reason why the pain comes back.[31] Teaching people with chronic low back pain how to use these muscles is recommended as part of a recovery program.[31]
Stop focusing on a specific diagnosis. Up to 85% of low back pain can be classified as "non-specific." This means that the origin of your pain cannot be localized to one specific structure or problem. While common diagnostic tests for low back pain can show the bones, discs, and joints with great detail, no test can tell the exact cause of your pain with 100% accuracy.
Key objects. If frequently used objects are too far out of arm’s reach, it can result in repeated twisting that can strain your lower back. To avoid this, keep things you use the most within easy reach. This could include your phone, stapler, pens, notepads, or anything else that gets regular use. If something is too large or heavy to keep near your keyboard, place it where you have to stand to get it to help you resist the urge to twist.
Melissa Conrad Stöppler, MD, is a U.S. board-certified Anatomic Pathologist with subspecialty training in the fields of Experimental and Molecular Pathology. Dr. Stöppler's educational background includes a BA with Highest Distinction from the University of Virginia and an MD from the University of North Carolina. She completed residency training in Anatomic Pathology at Georgetown University followed by subspecialty fellowship training in molecular diagnostics and experimental pathology.
Poor Sitting Posture: The correct position of your low back should have a slight forward curve called a lordosis. When you sit slouched, this lordosis straightens out-or even worse-reverses itself. This loss of the forward curve in your spine can cause increased pressure on the small shock absorbing discs in your back. This increased pressure can displace your discs and lead to low back pain. Your physical therapist can teach you the proper way to sit to decrease, eliminate, or prevent your back pain.
Treatment for greater trochanteric bursitis includes stretching and strengthening your IT band, hip abductors, and gluteal muscles, all while avoiding running on banked surfaces. Applying ice to the painful area for 15 minutes, three to four times per day can help, too. A cortisone injection may be beneficial if your injury is severe. Worsening pain should raise suspicion for a stress fracture, in which case you should see your doctor right away.
Arthritis. Osteoarthritis and rheumatoid arthritis are among the most common causes of hip pain, especially in older adults. Arthritis leads to inflammation of the hip joint and the breakdown of the cartilage that cushions your hip bones. The pain gradually gets worse. People with arthritis also feel stiffness and have reduced range of motion in the hip.
The lumbar (or lower back) region is made up of five vertebrae (L1–L5), sometimes including the sacrum. In between these vertebrae are fibrocartilaginous discs, which act as cushions, preventing the vertebrae from rubbing together while at the same time protecting the spinal cord. Nerves come from and go to the spinal cord through specific openings between the vertebrae, providing the skin with sensations and messages to muscles. Stability of the spine is provided by the ligaments and muscles of the back and abdomen. Small joints called facet joints limit and direct the motion of the spine.[30]
Epidural injections of steroid drugs are frequently used to treat sciatica, despite limited evidence for their effectiveness. Moreover, these treatments are based on the assumption that reducing local inflammation in the vertebral column will relieve pain, but an association between structural abnormalities, inflammation, and sciatica symptoms has not been clearly demonstrated. NINDS-funded researchers are using a new imaging technique that can detect inflammation to better understand what causes chronic sciatica pain and to provide evidence to inform treatment selection. 
Medications: A wide range of medications are used to treat acute and chronic low back pain. Some are available over the counter (OTC); others require a physician’s prescription. Certain drugs, even those available OTC, may be unsafe during pregnancy, may interact with other medications, cause side effects, or lead to serious adverse effects such as liver damage or gastrointestinal ulcers and bleeding. Consultation with a health care provider is advised before use. The following are the main types of medications used for low back pain:
As has been highlighted by research presented at the national meeting of the American College of Rheumatology, a very important aspect of the individual evaluation is the patient's own understanding and perception of their particular situation. British researchers found that those who believed that their symptoms had serious consequences on their lives and that they had, or treatments had, little control over their symptoms were more likely to have a poor outcome. This research points out to physicians the importance of addressing the concerns and perceptions that patients have about their condition during the initial evaluations.
A pinched nerve causes pain, numbness, or tingling in the affected area due to pressure on a nerve. Caral tunnel and sciatica are two examples of conditions caused by a pinched nerve. A pinched nerve is diagnosed by taking a patient history and performing a physical examination. Electromyography may be performed. Treatment for a pinched nerve depends on the underlying cause.
Other problems may occur along with low back pain. Chronic low back pain is associated with sleep problems, including a greater amount of time needed to fall asleep, disturbances during sleep, a shorter duration of sleep, and less satisfaction with sleep.[24] In addition, a majority of those with chronic low back pain show symptoms of depression[13] or anxiety.[17]
Disc degeneration remains a key cause of chronic low back pain and the pain often persists despite surgery. NIH-funded basic science and preclinical studies are investigating molecular-level mechanisms that cause discs in the spine to degenerate, as well as protective mechanisms involved in disc remodeling that may diminish with advancing age. Such studies may help identify future therapeutic strategies to block degenerative mechanisms or promote remodeling processes. NIH also is funding early research on stem cell approaches to promote disc regeneration and rejuvenate cells of the nucleus pulposus, the jelly-like substance in the center of intervertebral discs that loses water content as people age.

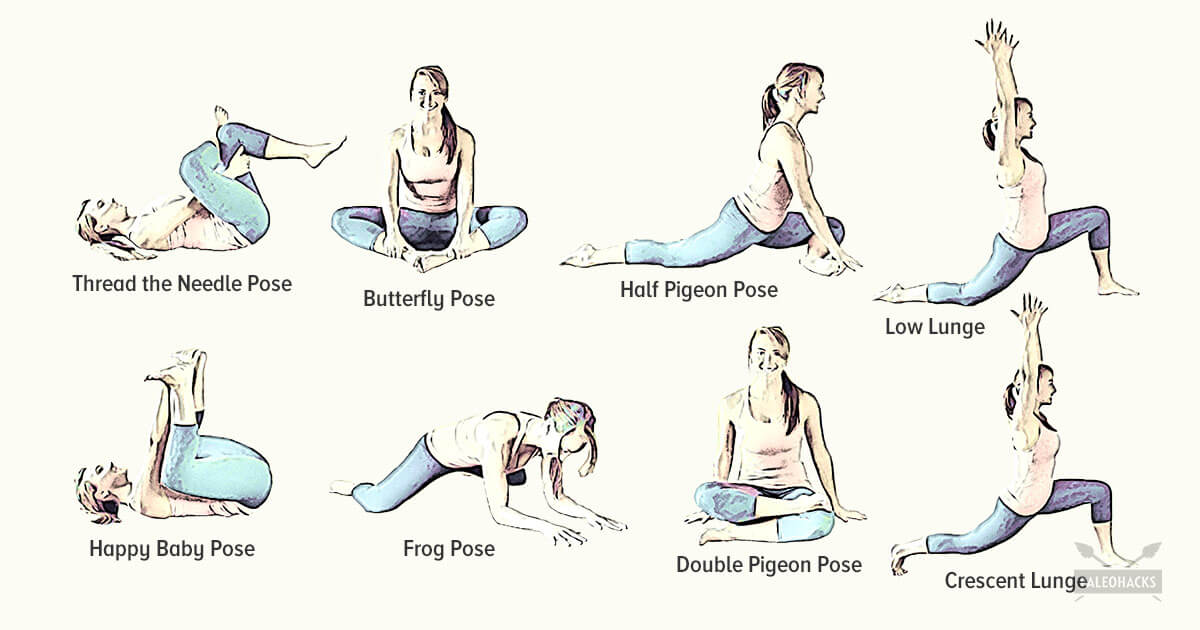
Sit on floor with knees bent and shins stacked with right leg on top. Use your hand to position right ankle on left knee. Ideally, the right knee will rest on the left thigh, but if your hips are tight, your right knee may point up toward the ceiling (overtime, as your hips become more open, your knee will lower). Keeping your hips squared to the front of the room, hinge at the hips and slowly walk hands slightly forward. If this is enough of a stretch, hold here, or fold your torso over your thighs to go deeper. Hold for at least 30 seconds, then repeat on opposite side.
Nonsteroidal anti-inflammatory drugs (NSAIDS) relieve pain and inflammation and include OTC formulations (ibuprofen, ketoprofen, and naproxen sodium). Several others, including a type of NSAID called COX-2 inhibitors, are available only by prescription. Long-term use of NSAIDs has been associated with stomach irritation, ulcers, heartburn, diarrhea, fluid retention, and in rare cases, kidney dysfunction and cardiovascular disease. The longer a person uses NSAIDs the more likely they are to develop side effects. Many other drugs cannot be taken at the same time a person is treated with NSAIDs because they alter the way the body processes or eliminates other medications.
Infection of the discs (septic discitis) and bone (osteomyelitis) is extremely rare. These conditions lead to localized pain associated with fever. The bacteria found when these tissues are tested with laboratory cultures include Staphylococcus aureus and Mycobacterium tuberculosis (TB bacteria). TB infection in the spine is called Pott's disease. These are each very serious conditions requiring long courses of antibiotics. The sacroiliac joints rarely become infected with bacteria. Brucellosis is a bacterial infection that can involve the sacroiliac joints and is usually transmitted in raw goat's milk.
Great exercises and stretches that can be easily done throughout the day to strengthen and loosen my hip flexors. i have very tight hip flexors so it's very helpful for me knowing these exercises and stretches. For those that want more info about exercises and stretches for hip flexors, i recommend the "unlock your hip flexors". It is a program that will show you many more exercises and stretches you can do. So check it out here
Most low back pain is acute, or short term, and lasts a few days to a few weeks. It tends to resolve on its own with self-care and there is no residual loss of function. The majority of acute low back pain is mechanical in nature, meaning that there is a disruption in the way the components of the back (the spine, muscle, intervertebral discs, and nerves) fit together and move.
Start in a runner’s lunge with right leg forward, right knee over right ankle and back leg straight. Walk right foot over toward left hand, then drop right shin and thigh to the floor, making sure to keep right knee in line with right hip. Allow left leg to rest on the floor with top of left foot facing down. Take a moment to square your hips to the front of the room. Hold here, or hinge at hips and lower torso toward floor, allowing head to rest on forearms. Hold for at least 30 seconds, then repeat on opposite side. You want to feel a moderate stretch in the outside of the right thigh, but if this pose hurts your knees or feels too uncomfortable, stick with Thread the Needle.

But moving is important for hip and knee OA. It causes your joints to compress and release, bringing blood flow, nutrients, and oxygen into the cartilage. “This can help prolong the function and longevity of your joints,” says Eric Robertson, DPT, a physical therapist and associate professor of clinical physical therapy at the University of Southern California.

When was the last time you got on your gym's abductor or adductor machine and got in a good workout? It's probably been a while. Both are machines that don't get a lot of use, and they are often the target of coaches' ridicule on those "useless gym moves we should all skip" lists. Perhaps rightly so, especially if you're hopping on those machines hoping for a slimming effect. 


