Degenerative Conditions: Sometimes, degenerative conditions that are the normal result of aging may cause your low back pain. Conditions like spinal stenosis, arthritis, or degenerative disc disease can all cause pain. Congenital conditions, like spondylolisthesis or scoliosis, can also cause your back pain. For most degenerative back problems, movement and exercise have been proven to be effective in treating these conditions. A visit to your physical therapist can help you determine the correct progression of back exercises for your specific condition.
Marvelously progressive, concise, and cogent guidelines for physicians on the treatment of low back pain. These guidelines almost entirely “get it right” in my opinion, and are completely consistent with recommendations I’ve been making for years on PainScience.com. They are particularly to be praised for strongly discouraging physicians from ordering imaging tests only “for patients with low back pain when severe or progressive neurologic deficits are present or when serious underlying conditions are suspected.”
The management of low back pain often includes medications for the duration that they are beneficial. With the first episode of low back pain the hope is a complete cure; however, if the problem becomes chronic, the goals may change to pain management and the recovery of as much function as possible. As pain medications are only somewhat effective, expectations regarding their benefit may differ from reality, and this can lead to decreased satisfaction.[13]

In both younger and older patients, vertebral fractures take weeks to heal with rest and pain relievers. Compression fractures of vertebrae associated with osteoporosis can also be treated with a procedure called vertebroplasty or kyphoplasty, which can help to reduce pain. In this procedure, a balloon is inflated in the compressed vertebra, often returning some of its lost height. Subsequently, a "cement" (methymethacrylate) is injected into the balloon and remains to retain the structure and height of the body of the vertebra. Pain is relieved as the height of the collapsed vertebra is restored.
^ Jump up to: a b c d American College of Occupational and Environmental Medicine (February 2014), "Five Things Physicians and Patients Should Question", Choosing Wisely: an initiative of the ABIM Foundation, American College of Occupational and Environmental Medicine, archived from the original on 11 September 2014, retrieved 24 February 2014, which cites
When intervertebral disks collapse and osteoarthritis develops, your body may respond by growing new bone in your facet joints to help support the vertebrae. Over time, this bone overgrowth (called spurs) can lead to a narrowing of the spinal canal. Osteoarthritis can also cause the ligaments that connect vertebrae to thicken, which can narrow the spinal canal.
Those are some great stretches! I own a personal training studio in Severna Park, Maryland. Majority of my clients have physical limitations – so it’s important for them to stay flexible. I send these to my clients and even do these exercises for myself. I highly recommend these stretches to anyone, even people without physical limitations. I love the fact these are actually videos and not just stretches because it’s so much easier for people to figure out how to perform the stretches. You guys are the real MVP!

Compressive pain is a result of pressure or irritation on the spinal cord, nerves that leave the spine. For example, if an intervertebral disc herniates (usually called a ruptured disc) and pushes into the spinal canal, it can cause problems with the nerve. Usually this pressure or irritation causes pain, numbness, and muscle weakness where the nerve travels.
When intervertebral disks collapse and osteoarthritis develops, your body may respond by growing new bone in your facet joints to help support the vertebrae. Over time, this bone overgrowth (called spurs) can lead to a narrowing of the spinal canal. Osteoarthritis can also cause the ligaments that connect vertebrae to thicken, which can narrow the spinal canal.
Brace your core and bend your knees to lower down into a split squat. Your left knee should ideally form a 90-degree angle so that your thigh is parallel to the ground, and your right knee is hovering above the floor. (Quick position check: your left foot should be stepped out far enough that you can do this without letting your left knee go past your left toes—if you can't, hop your left foot out a bit farther away from the bench.)
Iliopsoas syndrome, which is also called psoas syndrome or iliopsoas tendonitis, occurs when the iliopsoas muscles are injured. Lower back pain is the most common symptom; however, pain can also occur in the hip, thigh, or leg. The iliopsoas bursa, which is a fluid-filled sac located on the inside of the hip that reduces rubbing and friction, is also likely to become inflamed due to the proximity of the two structures. When this happens, the inflamed bursae will make it difficult to move.

The symptoms can also be classified by duration as acute, sub-chronic (also known as sub-acute), or chronic. The specific duration required to meet each of these is not universally agreed upon, but generally pain lasting less than six weeks is classified as acute, pain lasting six to twelve weeks is sub-chronic, and more than twelve weeks is chronic.[3] Management and prognosis may change based on the duration of symptoms.
Hi John, Thank you for the video and instructions. My question to you is that I’m schedule to have a reconstructive hip repair (Laberal tear) in July for my right hip and (second) and told that I have a tear in the right as well. I’ve been suffering from back pain too and know its because of the hips and my sitting because of work. If I can tolerate the exercise, would your recommend to do them? And if so, should I take it down from your suggested reps? I’ve been doing DDP Yoga for the last week and besides general soreness and some discomfort in my right hip, i’ve been able to make it through a full workout as well as do the core exercises. Your response would be greatly appreciated.
You’d think so. But consider this story of a motorcycle accident: many years ago, a friend hit a car that had pulled out from a side street. He flew over the car & landed on his head. Bystanders showed their ignorance of spinal fracture by, yikes, carelessly moving him. In fact, his thoracic spine was significantly fractured … yet the hospital actually refused to do an X-ray because he had no obvious symptoms of a spinal fracture. Incredible! The next day, a horrified orthopedic surgeon ordered an X-ray immediately, confirming the fracture & quite possibly saved him from paralysis.
Arthritis. Osteoarthritis and rheumatoid arthritis are among the most common causes of hip pain, especially in older adults. Arthritis leads to inflammation of the hip joint and the breakdown of the cartilage that cushions your hip bones. The pain gradually gets worse. People with arthritis also feel stiffness and have reduced range of motion in the hip.
The bones of the hip are supported by specific muscles. The strongest muscle in the body is actually one of the main flexors of the hip, it is called the iliopsoas muscle. It has two attachments to the inner part of the hip as well as the lower part of the back. This muscle is involved in iliopsoas tendinitis, iliopsoas bursitis, and is one of the most common causes of muscle pain that causes hip pain. The tendons attach the muscles to the bones and the ligaments attach bone to bone. Areas that are often susceptible to increased pressure are the tendons or the muscles attached to the bone, so that is another source of pain in iliopsoas tendinitis. The bursa are pockets of fluid that also protect the top part of the bone to prevent pressure on the bone. There are about 160 bursa in the body, and when they get irritated, it can develop into bursitis.
In diagnosing the causes of hip pain, it’s important to understand hip anatomy. The hip is basically a ball-and-socket joint similar to the shoulder joint and the arms. The hip joint is impressive in that it serves two factors, it is a support structure and also very flexible. Because it is a strong support structure, it tends to get injured. Because it’s very flexible, it similarly can be susceptible to injuries.
Medications: A wide range of medications are used to treat acute and chronic low back pain. Some are available over the counter (OTC); others require a physician’s prescription. Certain drugs, even those available OTC, may be unsafe during pregnancy, may interact with other medications, cause side effects, or lead to serious adverse effects such as liver damage or gastrointestinal ulcers and bleeding. Consultation with a health care provider is advised before use. The following are the main types of medications used for low back pain:

Epidural steroid injections are a commonly used short-term option for treating low back pain and sciatica associated with inflammation. Pain relief associated with the injections, however, tends to be temporary and the injections are not advised for long-term use. An NIH-funded randomized controlled trial assessing the benefit of epidural steroid injections for the treatment of chronic low back pain associated with spinal stenosis showed that long-term outcomes were worse among those people who received the injections compared with those who did not.
Premkumar et al present evidence that the traditional “red flags” for ominous causes of back pain can be quite misleading. The correlation between red flags and ominous diagnoses is poor, and prone to producing false negatives: that is, no red flags even when there is something more serious than unexplained pain going on. In a survey of almost 10,000 patients “the absence of red flag responses did not meaningfully decrease the likelihood of a red flag diagnosis.“ This is not even remotely a surprise to anyone who paid attention in back pain school, but it’s good to have some harder data on it.
Vertebroplasty and kyphoplasty are minimally invasive treatments to repair compression fractures of the vertebrae caused by osteoporosis. Vertebroplasty uses three-dimensional imaging to assist in guiding a fine needle through the skin into the vertebral body, the largest part of the vertebrae. A glue-like bone cement is then injected into the vertebral body space, which quickly hardens to stabilize and strengthen the bone and provide pain relief. In kyphoplasty, prior to injecting the bone cement, a special balloon is inserted and gently inflated to restore height to the vertebral structure and reduce spinal deformity.

Strengthening exercises, beyond general daily activities, are not advised for acute low back pain, but may be an effective way to speed recovery from chronic or subacute low back pain. Maintaining and building muscle strength is particularly important for persons with skeletal irregularities. Health care providers can provide a list of beneficial exercises that will help improve coordination and develop proper posture and muscle balance. Evidence supports short- and long-term benefits of yoga to ease chronic low back pain.
When was the last time you got on your gym's abductor or adductor machine and got in a good workout? It's probably been a while. Both are machines that don't get a lot of use, and they are often the target of coaches' ridicule on those "useless gym moves we should all skip" lists. Perhaps rightly so, especially if you're hopping on those machines hoping for a slimming effect.

"As compared to a conventional deadlift, the sumo allows for greater recruitment of the adductors and a more stabilizing emphasis for the abductors," says Lindsey Cormack, a competitive powerlifter and CrossFit trainer. "Training sumo may feel less stable at first, but the balance requirement is what allows you to effectively train both the abductors and adductors."
Epidural steroid injections are most commonly used in situations of radicular pain, which is a radiating pain that is transmitted away from the spine by an irritated spinal nerve. Irritation of a spinal nerve in the low back (lumbar radiculopathy) causes pain that goes down the leg. Epidural injections are also used to treat nerve compression in the neck (cervical spine), referred to as cervical radiculopathy, which causes pain.
^ Dubinsky, R. M.; Miyasaki, J. (2009). "Assessment: Efficacy of transcutaneous electric nerve stimulation in the treatment of pain in neurologic disorders (an evidence-based review): Report of the Therapeutics and Technology Assessment Subcommittee of the American Academy of Neurology". Neurology. 74 (2): 173–6. doi:10.1212/WNL.0b013e3181c918fc. PMID 20042705.

Pain in the hip can result from a number of factors. Sometimes diseases that affect other joints in the body, such as the inflammation resulting from arthritis, can be the cause of pain in the hip. Depending upon the cause of hip pain, the pain may occur when walking, running, or engaging in activity. Trochanteric bursitis is the most common type of hip bursitis and causes pain at the point of the hip.
Stop focusing on a specific diagnosis. Up to 85% of low back pain can be classified as "non-specific." This means that the origin of your pain cannot be localized to one specific structure or problem. While common diagnostic tests for low back pain can show the bones, discs, and joints with great detail, no test can tell the exact cause of your pain with 100% accuracy. 
Bleeding in the pelvis is rare without significant trauma and is usually seen in patients who are taking blood-thinning medications, such as warfarin (Coumadin). In these patients, a rapid-onset sciatica pain can be a sign of bleeding in the back of the pelvis and abdomen that is compressing the spinal nerves as they exit to the lower extremities. Infection of the pelvis is infrequent but can be a complication of conditions such as diverticulosis, Crohn's disease, ulcerative colitis, pelvic inflammatory disease with infection of the Fallopian tubes or uterus, and even appendicitis. Pelvic infection is a serious complication of these conditions and is often associated with fever, lowering of blood pressure, and a life-threatening state.
Simply stand up straight with your feet about shoulder-width apart. Slowly bend your knees and hips, lowering yourself until your knees obscure your toes or you achieve a 90 degree angle. Hold for a count of 5 and then gently resume your original position. This can be a tough one so again, don’t overdo it and hold on to a table if you need a little extra support! Try to repeat between 5-10 times.

Physician specialties that evaluate and treat low back pain range from generalists to subspecialists.These specialties include emergency medicine physicians, general medicine, family medicine, internal medicine, gynecology, spine surgeons (orthopaedics and neurosurgery), rheumatology, pain management, and physiatry. Other health care providers for low back pain include physical therapists, chiropractors, massage therapists, psychologists, and acupuncturists.
In both younger and older patients, vertebral fractures take weeks to heal with rest and pain relievers. Compression fractures of vertebrae associated with osteoporosis can also be treated with a procedure called vertebroplasty or kyphoplasty, which can help to reduce pain. In this procedure, a balloon is inflated in the compressed vertebra, often returning some of its lost height. Subsequently, a "cement" (methymethacrylate) is injected into the balloon and remains to retain the structure and height of the body of the vertebra. Pain is relieved as the height of the collapsed vertebra is restored.

Behavioral therapy may be useful for chronic pain.[16] There are several types available, including operant conditioning, which uses reinforcement to reduce undesirable behaviors and increase desirable behaviors; cognitive behavioral therapy, which helps people identify and correct negative thinking and behavior; and respondent conditioning, which can modify an individual's physiological response to pain.[17] The benefit however is small.[91] Medical providers may develop an integrated program of behavioral therapies.[17] The evidence is inconclusive as to whether mindfulness-based stress reduction reduces chronic back pain intensity or associated disability, although it suggests that it may be useful in improving the acceptance of existing pain.[92][93]
Prolonged sitting and activities like running or cycling can lead to tight hip flexor muscles and a variety of skeletal imbalances. Think: if you only cycle for exercise, certain muscles in your legs will get stronger (in a lot of cases you overwork these muscles) yet your core and outer hip muscles might get weaker from lack of engagement. So what? Well, these muscle imbalances often lead to skeletal imbalances and injuries down the line. If you have particularly tight hip flexors, your body will start to create an anterior pull on the pelvis (anterior pelvic tilt). You can identify an anterior pelvic tilt if your belly protrudes slightly in the front while your butt sticks out in the back (what some people refer to as “duck butt”).

^ Jump up to: a b Chou R, Qaseem A, Owens DK, Shekelle P, Clinical Guidelines Committee of the American College of Physicians (1 February 2011). "Diagnostic imaging for low back pain: advice for high-value health care from the American College of Physicians". Annals of Internal Medicine. 154 (3): 181–9. doi:10.7326/0003-4819-154-3-201102010-00008. PMID 21282698.
Initial management with non–medication based treatments is recommended.[6] NSAIDs are recommended if these are not sufficiently effective.[6] Normal activity should be continued as much as the pain allows.[2] Medications are recommended for the duration that they are helpful.[13] A number of other options are available for those who do not improve with usual treatment. Opioids may be useful if simple pain medications are not enough, but they are not generally recommended due to side effects.[4][13] Surgery may be beneficial for those with disc-related chronic pain and disability or spinal stenosis.[14][15] No clear benefit has been found for other cases of non-specific low back pain.[14] Low back pain often affects mood, which may be improved by counseling or antidepressants.[13][16] Additionally, there are many alternative medicine therapies, including the Alexander technique and herbal remedies, but there is not enough evidence to recommend them confidently.[17] The evidence for chiropractic care[18] and spinal manipulation is mixed.[17][19][20][21]
Along with mobility and strength exercises, it's a good idea to do some flexibility work on a regular basis, especially as the season progresses and you start increasing your training mileage. Yoga is a great option—variations of hip openers and other poses can really help the overall function of your hips. The following stretches will help increase flexibility in your hips.
People understandably assume that the worst back pain is the scariest. In fact, pain intensity is a poor indicator of back pain ominousness,10 and some of the worst causes are actually the least painful (especially in the early stages). For instance, someone could experience the symptoms of cauda equinae syndrome, and be in real danger of a serious and permanent injury to their spine, but have surprisingly little pain — even none at all in some cases!
But how can you tell? It can be tricky. This is a concise, readable guide to symptoms that need better-safe-than-sorry investigation with your doctor. (It’s basically just a plain English version of clinical guidelines for doctors.9) In other words, this article explains the difference between “dangerous” and “just painful” as clearly as possible. Tables, checklists, and examples ahead.
The iliopsoas muscles are a group of two muscles—the psoas muscle and the iliacus muscle—located toward the front of the inner hip. The psoas muscles, in particular, is located in the lumbar (lower) region of the spine and extends through the pelvis to the femur. The iliopsoas muscles are the primary hip flexors, pulling the knee up off the ground when it contracts. Because the psoas muscle is also connected to the spine, it contributes to upright posture, assists in lumbar spine movement, and influences the spine’s curve.
Kneel on your mat with thighs perpendicular to the floor and tops of of your feet facing down. Place a yoga block between your feet. Bring your inner knees together. Slide your feet apart so they are slightly wider than your hips, and press the tops of your feet evenly into the mat. Slowly sit down on the yoga block. Use your hands to turn the top of your thighs inward. Allow the backs of your hands to rest on your thighs. Hold for at least 30 seconds.
Start in a runner’s lunge, right leg forward with knee over ankle and left knee on ground with top of your foot flat on the mat. Slowly lift torso and rest hands lightly on right thigh. Lean hips forward slightly, keeping right knee behind toes, and feel the stretch in the left hip flexor. Hold here, or for a deeper stretch, raise arms overhead, biceps by ears. Hold for at least 30 seconds, then repeat on opposite side.
Pain in the front of the joint—where the leg attaches to the trunk—is typically caused by hip joint problems. You may also feel pain associated with a hip injury in the lower part of your glutes and the top of the back of your thigh. Other symptoms include the inability to move the leg at the hip, inability to put weight on one leg due to pain at the hip, or swelling around the joint. As runners, you may also experience pain in the hipo joint only when running due to a hip injury.
If certain activities or overuse are causing hip pain, stop those that aggravate the discomfort and talk to your doctor. Excess weight can put pressure on the hip joint, so losing the pounds can provide relief and help you avoid further problems. Some causes of hip pain, such as fractures or hernias, may need surgical repairs. If your hip pain persists, talk to your doctor about the possible causes and treatments.
For strains and tendinitis at the top of the hamstrings, treatment is the same as that used for hip flexor problems. Hamstring stretching and strengthening—such as side lunges, inward leg raises, and backward leg raises—is important. Deep tissue massage may also be beneficial, but in general, this is a difficult problem that usually takes a while to resolve.
Sciatica is a form of radiculopathy caused by compression of the sciatic nerve, the large nerve that travels through the buttocks and extends down the back of the leg. This compression causes shock-like or burning low back pain combined with pain through the buttocks and down one leg, occasionally reaching the foot. In the most extreme cases, when the nerve is pinched between the disc and the adjacent bone, the symptoms may involve not only pain, but numbness and muscle weakness in the leg because of interrupted nerve signaling. The condition may also be caused by a tumor or cyst that presses on the sciatic nerve or its roots.

There is a significant overlap of nerve supply to many of the discs, muscles, ligaments, and other spinal structures, and it can be difficult for the brain to accurately sense which is the cause of the pain. For example, a degenerated or torn lumbar disc can feel the same as a pulled muscle – both creating inflammation and painful muscle spasm in the same area. Muscles and ligaments heal rapidly, while a torn disc may or may not. The time course of pain helps determine the cause.

This Web site provides general educational information on health-related issues and provides access to health-related resources for the convenience of our users. This site and its health-related information and resources are not a substitute for professional medical advice or for the care that patients receive from their physicians or other health care providers.

Epidural injections of steroid drugs are frequently used to treat sciatica, despite limited evidence for their effectiveness. Moreover, these treatments are based on the assumption that reducing local inflammation in the vertebral column will relieve pain, but an association between structural abnormalities, inflammation, and sciatica symptoms has not been clearly demonstrated. NINDS-funded researchers are using a new imaging technique that can detect inflammation to better understand what causes chronic sciatica pain and to provide evidence to inform treatment selection.

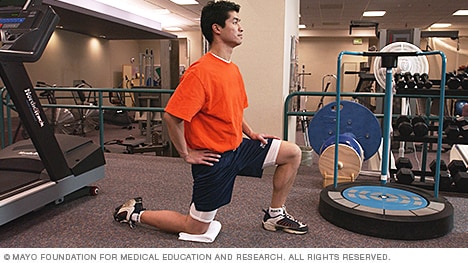
Apply the above concept to your hips. When you sit, your hips are in a "flexed" position. Therefore, the muscles that flex your hips are in a shortened state. You probably spend at least a third of your day sitting down. Think about how much time those hip flexor muscles stay shortened. A lot. Over time, they become tighter and tighter until you look like the old man in the picture. So unless you want to look like that, perform the stretches shown below. 
Pregnancy symptoms can vary from woman to woman, and not all women experience the same symptoms. When women do experience pregnancy symptoms they may include symptoms include missed menstrual period, mood changes, headaches, lower back pain, fatigue, nausea, breast tenderness, and heartburn. Signs and symptoms in late pregnancy include leg swelling and shortness of breath. Options for relief of pregnancy symptoms include exercise, diet, and other lifestyle changes.
Sciatica is a form of radiculopathy caused by compression of the sciatic nerve, the large nerve that travels through the buttocks and extends down the back of the leg. This compression causes shock-like or burning low back pain combined with pain through the buttocks and down one leg, occasionally reaching the foot. In the most extreme cases, when the nerve is pinched between the disc and the adjacent bone, the symptoms may involve not only pain, but numbness and muscle weakness in the leg because of interrupted nerve signaling. The condition may also be caused by a tumor or cyst that presses on the sciatic nerve or its roots.
Luckily, you don’t have to quit your day job or forgo spin class to loosen them up. Simply stretching those hips can get your body back in alignment, increase your mobility (and thus your exercise performance) and maybe even ease pesky back pain, Moore says. “Given the amount of time we sit [each] day and the stress we put our bodies under, hip-opening moves are a necessary party of our daily routine.”
Just because your hip flexor region feels sore doesn’t necessarily mean the muscles there are tight — in fact, they might need strengthening. This is where that sports science debate we mentioned earlier comes into play. It’s important to identify whether you’re tight or if the muscles are weak. Again, the Thomas Test will help you identify if you’re maybe stretching something that actually needs strengthening.
Back “spasms” are a largely a myth — there’s no such thing a sustained painful contractions of muscles in otherwise healthy people (see Cramps, Spasms, Tremors & Twitches) — but the kernel of truth in the idea of “spasms” may be the idea of trigger points, which are hypothetical “micro cramps,” tiny patches of painfully contracting muscle. Although this idea is controversial, it is nevertheless one of the most likely explanations for common aches and pains that mostly stick to one area (especially the back) and have no other obvious cause. See Back Pain & Trigger Points. BACK TO TEXT

"As compared to a conventional deadlift, the sumo allows for greater recruitment of the adductors and a more stabilizing emphasis for the abductors," says Lindsey Cormack, a competitive powerlifter and CrossFit trainer. "Training sumo may feel less stable at first, but the balance requirement is what allows you to effectively train both the abductors and adductors."
Bleeding in the pelvis is rare without significant trauma and is usually seen in patients who are taking blood-thinning medications, such as warfarin (Coumadin). In these patients, a rapid-onset sciatica pain can be a sign of bleeding in the back of the pelvis and abdomen that is compressing the spinal nerves as they exit to the lower extremities. Infection of the pelvis is infrequent but can be a complication of conditions such as diverticulosis, Crohn's disease, ulcerative colitis, pelvic inflammatory disease with infection of the Fallopian tubes or uterus, and even appendicitis. Pelvic infection is a serious complication of these conditions and is often associated with fever, lowering of blood pressure, and a life-threatening state.
Men and women are equally affected by low back pain, which can range in intensity from a dull, constant ache to a sudden, sharp sensation that leaves the person incapacitated. Pain can begin abruptly as a result of an accident or by lifting something heavy, or it can develop over time due to age-related changes of the spine. Sedentary lifestyles also can set the stage for low back pain, especially when a weekday routine of getting too little exercise is punctuated by strenuous weekend workout.
^ Dubinsky, R. M.; Miyasaki, J. (2009). "Assessment: Efficacy of transcutaneous electric nerve stimulation in the treatment of pain in neurologic disorders (an evidence-based review): Report of the Therapeutics and Technology Assessment Subcommittee of the American Academy of Neurology". Neurology. 74 (2): 173–6. doi:10.1212/WNL.0b013e3181c918fc. PMID 20042705.
Running: Running may be good for boosting your cardiovascular health but it can be very strenuous if you have hip pain. The impact can upset your hip joints so instead focus on other forms of exercise. Walking is still a good option for hip pain if you really feel like working out in the great outdoors or you could instead try some strengthening exercises from the comfort of your own home.

Spinal fusion is used to strengthen the spine and prevent painful movements in people with degenerative disc disease or spondylolisthesis (following laminectomy). The spinal disc between two or more vertebrae is removed and the adjacent vertebrae are “fused” by bone grafts and/or metal devices secured by screws. The fusion can be performed through the abdomen, a procedure known as an anterior lumbar interbody fusion, or through the back, called posterior fusion. Spinal fusion may result in some loss of flexibility in the spine and requires a long recovery period to allow the bone grafts to grow and fuse the vertebrae together. Spinal fusion has been associated with an acceleration of disc degeneration at adjacent levels of the spine.
There are many causes of hip joint pain. Some hip pain is temporary, while other hip pain can be long-standing or chronic. Causes of hip pain include arthritis, inflammatory and noninflammatory arthritis, fracture, sprain, infectious arthritis (septic arthritis), avascular necrosis, Gaucher's disease, sciatica, muscle strain, iliotibial band syndrome (IT band syndrome), and hematoma.
Mechanical pain. By far the most common cause of lower back pain, mechanical pain (axial pain) is pain primarily from the muscles, ligaments, joints (facet joints, sacroiliac joints), or bones in and around the spine. This type of pain tends to be localized to the lower back, buttocks, and sometimes the top of the legs. It is usually influenced by loading the spine and may feel different based on motion (forward/backward/twisting), activity, standing, sitting, or resting.
How to do it: Stand with your feet together, holding dumbbells by your sides. Take a wide step out to your right and lower into a side lunge, reaching dumbbells on either side of right leg [as shown]. Bend your left knee and shift your weight into both legs, into a wide squat position, reaching the dumbbells to floor in front of you, then extend your right leg and shift your weight to the left, moving into a side lunge with your left leg.
I had compromised range of motion in my hips. I am a runner and I couldn’t increase my speed. Using this program – http://certifiedtreatment.com/hipflexors I adjusted my back and relieved the pain the tightness in my hips and lower back which allowed me to run harder and longer. Not only do I have less pain on a daily basis, but I also have more energy and stamina when I run. I find myself with better movement and sleep, and I have maximized my performance.
Deanna is an ACE® certified personal trainer, Balanced Body® Pilates instructor, and NASM® Fitness Nutrition Specialist. She is passionate about inspiring others to lead a healthier lifestyle through fun workouts and healthy food. When she’s not creating new workouts and recipes for her blog The Live Fit Girls she enjoys running with her two dogs and traveling.
Discography may be used when other diagnostic procedures fail to identify the cause of pain. This procedure involves the injection of a contrast dye into a spinal disc thought to be causing low back pain. The fluid’s pressure in the disc will reproduce the person’s symptoms if the disc is the cause. The dye helps to show the damaged areas on CT scans taken following the injection. Discography may provide useful information in cases where people are considering lumbar surgery or when their pain has not responded to conventional treatments.
^ Jump up to: a b c d e f Qaseem, A; Wilt, TJ; McLean, RM; Forciea, MA; Clinical Guidelines Committee of the American College of, Physicians. (4 April 2017). "Noninvasive Treatments for Acute, Subacute, and Chronic Low Back Pain: A Clinical Practice Guideline From the American College of Physicians". Annals of Internal Medicine. 166 (7): 514–530. doi:10.7326/M16-2367. PMID 28192789.
Kidneys — The kidneys are a matched pair. One painful kidney can cause back pain on one side or the other. Kidney pain can feel like back pain, and may occur on only one side. It is usually quite lateral, and just barely low enough to qualify as “low” back pain. However, when kidney stones descend through the ureters, they can cause (terrible) pain in the low back. Kidney stone pain is often so severe and develops so rapidly that it isn’t mistaken for a back pain problem.
We’re confident you’ll love your Onnit supplements. If the product doesn't perform for you, however, we’re not gonna play games with you. Order any of our entry size supplements, and if you don’t like it, you can keep it! Notify our team, telling us why it wasn't a fit for you, and we’ll get you a refund right there on the spot - no return necessary. We just ask that you try it out for at least two weeks to give it a fair shot.
Start in a runner’s lunge, right leg forward with knee over ankle and left knee on ground with top of your foot flat on the mat. Slowly lift torso and rest hands lightly on right thigh. Lean hips forward slightly, keeping right knee behind toes, and feel the stretch in the left hip flexor. Hold here, or for a deeper stretch, raise arms overhead, biceps by ears. Hold for at least 30 seconds, then repeat on opposite side.
Just because your hip flexor region feels sore doesn’t necessarily mean the muscles there are tight — in fact, they might need strengthening. This is where that sports science debate we mentioned earlier comes into play. It’s important to identify whether you’re tight or if the muscles are weak. Again, the Thomas Test will help you identify if you’re maybe stretching something that actually needs strengthening.
The side of the pain on its own doesn’t tell us much, and most of the one-sided sources of pain are viscera that usually cause abdominal pain instead of back pain, or in addition to it. In other words, the only reason to worry about right or left lower back pain is if it is otherwise worrisome: if you have other red flags or significant non-back symptoms.
Key objects. If frequently used objects are too far out of arm’s reach, it can result in repeated twisting that can strain your lower back. To avoid this, keep things you use the most within easy reach. This could include your phone, stapler, pens, notepads, or anything else that gets regular use. If something is too large or heavy to keep near your keyboard, place it where you have to stand to get it to help you resist the urge to twist.
Talmage, J; Belcourt, R; Galper, J; et al. (2011). "Low back disorders". In Kurt T. Hegmann. Occupational medicine practice guidelines : evaluation and management of common health problems and functional recovery in workers (3rd ed.). Elk Grove Village, IL: American College of Occupational and Environmental Medicine. pp. 336, 373, 376–377. ISBN 978-0615452272.
Physician specialties that evaluate and treat low back pain range from generalists to subspecialists.These specialties include emergency medicine physicians, general medicine, family medicine, internal medicine, gynecology, spine surgeons (orthopaedics and neurosurgery), rheumatology, pain management, and physiatry. Other health care providers for low back pain include physical therapists, chiropractors, massage therapists, psychologists, and acupuncturists.
Stand tall with your hips square and bend your right knee, bringing your foot towards your bum. Grab the right foot with your right hand and actively pull the foot closer to your glutes. As you do this, send the right knee down towards the ground and keep both knees together. squeeze your butt to promote a posterior pelvic tilt and hold — then switch sides.


