Disk tear. Small tears to the outer part of the disk (annulus) sometimes occur with aging. Some people with disk tears have no pain at all. Others can have pain that lasts for weeks, months, or even longer. A small number of people may develop constant pain that lasts for years and is quite disabling. Why some people have pain and others do not is not well understood.
Bone scans are used to detect and monitor infection, fracture, or disorders in the bone. A small amount of radioactive material is injected into the bloodstream and will collect in the bones, particularly in areas with some abnormality. Scanner-generated images can be used to identify specific areas of irregular bone metabolism or abnormal blood flow, as well as to measure levels of joint disease.

People routinely have no pain despite the presence of obvious arthritic degeneration, herniated discs, and other seemingly serious structural problems like stenosis and spondylolistheses. This surprising contradiction has been made clear by a wide variety of research over the years, but the most notable in recent history is Brinjikji 2015. There are painful spinal problems, of course — which was also shown by Brinjikji et al in a companion paper — but they are mostly more rare and unpredictable than most people suspect, and there are many fascinating examples of people who “should” be in pain but are not, and vice versa. Spinal problems are only one of many ingredients in back pain. BACK TO TEXT
We implement a variety of security measures to maintain the safety of your personal information when you place an order or enter, submit, or access any information on our website. We incorporate physical, electronic, and administrative procedures to safeguard the confidentiality of your personal information, including Secure Sockets Layer (SSL) for the encryption of all financial transactions through the website. We use industry-standard, 256bit SSL encryption to protect your personal information online, and we also take several steps to protect your personal information in our facilities. For example, when you visit the website, you access servers that are kept in a secure physical environment, behind a locked cage and a hardware firewall. After a transaction, your credit card information is not stored on our servers.

Brace your core and bend your knees to lower down into a split squat. Your left knee should ideally form a 90-degree angle so that your thigh is parallel to the ground, and your right knee is hovering above the floor. (Quick position check: your left foot should be stepped out far enough that you can do this without letting your left knee go past your left toes—if you can't, hop your left foot out a bit farther away from the bench.)
Why is back pain still a huge problem? Maybe this: “It is extremely difficult to alter the potentially disabling belief among the lay public that low back pain has a structural mechanical cause. An important reason for this is that this belief continues to be regularly reinforced by the conditions of care of a range of ‘hands-on’ providers, for whom idiosyncratic variations of that view are fundamental to their professional existence.”
How to: Sit on the floor with knees bent so that your right shin is positioned in front of you, your left shin behind you and your left hip dropped all of the way to the floor (a). Inhale and press your left hip forward until you feel a stretch in the front of your hip (b). Exhale and press left hip back to the floor. That’s one rep (c). Complete six to eight reps, working each time to increase your range of motion. Repeat on the opposite side.
Traction involves the use of weights and pulleys to apply constant or intermittent force to gradually “pull” the skeletal structure into better alignment. Some people experience pain relief while in traction, but that relief is usually temporary. Once traction is released the back pain tends to return. There is no evidence that traction provides any longterm benefits for people with low back pain.

Deanna is an ACE® certified personal trainer, Balanced Body® Pilates instructor, and NASM® Fitness Nutrition Specialist. She is passionate about inspiring others to lead a healthier lifestyle through fun workouts and healthy food. When she’s not creating new workouts and recipes for her blog The Live Fit Girls she enjoys running with her two dogs and traveling.

It is sometimes hard for an aggressive athlete to consider changing training schedules. It is also hard to accept the fact that a serious disease may exist. All athletes who suffer from low back pain should seek medical advice. Some situations might require reducing or stopping athletic activity until the problem is resolved. The body's ability to be active is worth preserving.
Along with mobility and strength exercises, it's a good idea to do some flexibility work on a regular basis, especially as the season progresses and you start increasing your training mileage. Yoga is a great option—variations of hip openers and other poses can really help the overall function of your hips. The following stretches will help increase flexibility in your hips.
When hip pain comes from muscles, tendons, or ligament injuries, it typically come from overuse syndromes. This can come from overusing the strongest hip muscles in the body such as iliopsoas tendinitis; it can come from tendon and ligament irritations, which typically are involved in snapping hip syndrome. It can come from within the joint, which is more characteristic of hip osteoarthritis. Each of these types of pain present in slightly different ways, which is then the most important part in diagnosing what the cause is by doing a good physical examination.
The hip is a basic ball-and-socket joint. The ball is the femoral head—a knob on the top of the thigh bone—and the socket is an indentation in the pelvic bone. There is cartilage lining the joint (called the labrum) and ligaments that attach the pelvic and thigh bones. Numerous muscles attach around the hip, too, moving the joint through the basic motions of flexion (bending), extension (extending the leg behind you), abduction (lifting the leg away from the body), adduction (moving the leg inward), internal rotation, and external rotation.

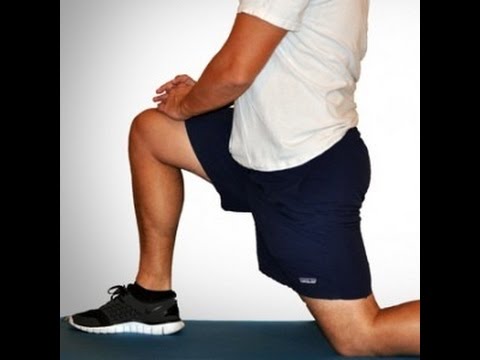
Stretching the hip muscles that sit on top of the bursae, part of the lining in your hip joint, can give you some relief from bursitis pain. Kneel on the leg that's giving you the pain, holding on to something sturdy for balance. Tilt your pelvis forward, tightening your gluteus muscles (the muscles in your buttocks). Then lean away from the side of your hip that hurts, for instance to the left if you're kneeling on your right knee. You should feel a stretch from the top of your hip bone down the side of your leg to your knee, Humphrey says. Hold the stretch for 30 seconds and repeat once or twice.
People routinely have no pain despite the presence of obvious arthritic degeneration, herniated discs, and other seemingly serious structural problems like stenosis and spondylolistheses. This surprising contradiction has been made clear by a wide variety of research over the years, but the most notable in recent history is Brinjikji 2015. There are painful spinal problems, of course — which was also shown by Brinjikji et al in a companion paper — but they are mostly more rare and unpredictable than most people suspect, and there are many fascinating examples of people who “should” be in pain but are not, and vice versa. Spinal problems are only one of many ingredients in back pain. BACK TO TEXT
Take nonprescription pain medicine, such as acetaminophen, ibuprofen, or naproxen. Read the label and take as directed. Nonsteroidal anti-inflammatory medicines (NSAIDs), such as ibuprofen or naproxen, may cause stomach bleeding and other problems. These risks increase with age. Unless recommended by your healthcare provider, do not take an NSAID for more than 10 days.

Start kneeling on your mat with knees hip-width apart and hips directly over knees. Press your shins and the tops of your feet into the mat. Bring your hands to your low back, fingers pointing down, and rest palms above glutes. Inhale and lift your chest, and then slowly start to lean your torso back. From here, bring your right hand to rest on your right heel and then your left hand to your left heel. (If you can't reach your heels, turn your toes under; it will be easier to reach your heels in this modification.) Press your thighs forward so they are perpendicular to the floor. Keep your head in a relatively neutral position or, if it doesn't strain your neck, drop it back. Hold for 30 seconds. To come out of the pose, bring your hands to your hips and slowly, leading with your chest, lift your torso as you press the thighs down toward the floor.

With the stakes so high, doesn’t it make sense to do all you can to strengthen and protect your hips? Even if you have arthritis in a hip — the reason for 8 in 10 replacements — you may be able to manage pain with exercise. In a 2017 pilot study published in the Journal of Osteoporosis, women 65 and older who exercised three times a week in a supervised 12-week program reduced arthritic hip pain by over 30 percent, with similar gains in strength, and joint range of motion. The four exercises here will fortify the muscles that surround and support your hips, says trainer Robert Linkul, owner of Be Stronger Fitness in Sacramento, Calif. He advises doing these simple moves, two to three sets of five to 10 reps each, three times a week. Compare how you feel after three weeks.
Imaging is indicated when there are red flags, ongoing neurological symptoms that do not resolve, or ongoing or worsening pain.[5] In particular, early use of imaging (either MRI or CT) is recommended for suspected cancer, infection, or cauda equina syndrome.[5] MRI is slightly better than CT for identifying disc disease; the two technologies are equally useful for diagnosing spinal stenosis.[5] Only a few physical diagnostic tests are helpful.[5] The straight leg raise test is almost always positive in those with disc herniation.[5] Lumbar provocative discography may be useful to identify a specific disc causing pain in those with chronic high levels of low back pain.[41] Similarly, therapeutic procedures such as nerve blocks can be used to determine a specific source of pain.[5] Some evidence supports the use of facet joint injections, transforminal epidural injections and sacroilliac injections as diagnostic tests.[5] Most other physical tests, such as evaluating for scoliosis, muscle weakness or wasting, and impaired reflexes, are of little use.[5] 
Pregnancy commonly leads to low back pain by mechanically stressing the lumbar spine (changing the normal lumbar curvature) and by the positioning of the baby inside of the abdomen. Additionally, the effects of the female hormone estrogen and the ligament-loosening hormone relaxin may contribute to loosening of the ligaments and structures of the back. Pelvic-tilt exercises and stretches are often recommended for relieving this pain. Women are also recommended to maintain physical conditioning during pregnancy according to their doctors' advice. Natural labor can also cause low back pain.
Hip hikers (also known as the pelvic drop) are great exercises to get your gluteal muscles working in a weight bearing position. To do the exercise, stand sideways with one foot on a step and the other hanging off. Keeping both knees straight, lower down your pelvis on one side so your foot moves toward the floor. Both knees should remain straight; the motion should come from your hip joint. Once your pelvis is lowered down, slowly raise it back up to the starting position. Repeat the exercise for 10 repetitions.
Nonsteroidal anti-inflammatory drugs (NSAIDS) relieve pain and inflammation and include OTC formulations (ibuprofen, ketoprofen, and naproxen sodium). Several others, including a type of NSAID called COX-2 inhibitors, are available only by prescription. Long-term use of NSAIDs has been associated with stomach irritation, ulcers, heartburn, diarrhea, fluid retention, and in rare cases, kidney dysfunction and cardiovascular disease. The longer a person uses NSAIDs the more likely they are to develop side effects. Many other drugs cannot be taken at the same time a person is treated with NSAIDs because they alter the way the body processes or eliminates other medications.
Stretching is your next move, but not just any stretches. “Before your workout, you want to go for dynamic stretches, or stretches that put the joint through a full range of motion,” says Lefkowith. Moves like squats and lunges will get your muscles fired up (especially if you focus on squeezing your butt at the top of those squats), says Lefkowith.
A healthy diet is important for a number of reasons when you have lower back pain. First, eating well can help you maintain a healthy weight. Excess weight puts extra strain on your lower back, adding to your pain. Second, a diet that’s high in key nutrients can help promote bone growth and keep your bones strong. These must-have nutrients include:
Pain is generally an unpleasant feeling in response to an event that either damages or can potentially damage the body's tissues. There are four main steps in the process of feeling pain: transduction, transmission, perception, and modulation.[12] The nerve cells that detect pain have cell bodies located in the dorsal root ganglia and fibers that transmit these signals to the spinal cord.[33] The process of pain sensation starts when the pain-causing event triggers the endings of appropriate sensory nerve cells. This type of cell converts the event into an electrical signal by transduction. Several different types of nerve fibers carry out the transmission of the electrical signal from the transducing cell to the posterior horn of spinal cord, from there to the brain stem, and then from the brain stem to the various parts of the brain such as the thalamus and the limbic system. In the brain, the pain signals are processed and given context in the process of pain perception. Through modulation, the brain can modify the sending of further nerve impulses by decreasing or increasing the release of neurotransmitters.[12]
If your hips are killing you, you probably spend a lot of time sitting – in the car, at work, on that spinning seat – which puts your hips in near-constant “flexion”, says Cori Lefkowith, NASM-certified personal trainer and owner of Redefining Strength in Orange County, California. Even running involves a repetitive flexion movement that can cause pain.
The diagnosis of low back pain involves a review of the history of the illness and underlying medical conditions as well as a physical examination. It is essential that a complete story of the back pain be reviewed including injury history, aggravating and alleviating conditions, associated symptoms (fever, numbness, tingling, incontinence, etc.), as well as the duration and progression of symptoms. Aside from routine abdomen and extremity evaluations, rectal and pelvic examinations may eventually be required as well. Further tests for diagnosis of low back pain can be required including blood and urine tests, plain film X-ray tests, CAT scanning, MRI scanning, bone scanning, and tests of the nerves such as electromyograms (EMG) and nerve conduction velocities (NCV).
This information is not designed to replace a physician's independent judgment about the appropriateness or risks of a procedure for a given patient. Always consult your doctor about your medical conditions or back problem. SpineUniverse does not provide medical advice, diagnosis or treatment. Use of the SpineUniverse.com site is conditional upon your acceptance of our User Agreement

When I do a deep knee bend like a sumo squat I get a popping in the outside of my left knee. It feels like a big tendon or ligament is slipping per something. It isn’t painful peer se but I’m afraid if I do it a lot it will be. Is that a relatively common symptom for a guy with tight flexors, it bands, etc? Should I just push through it or have it checked out?
Prolonged sitting and activities like running or cycling can lead to tight hip flexor muscles and a variety of skeletal imbalances. Think: if you only cycle for exercise, certain muscles in your legs will get stronger (in a lot of cases you overwork these muscles) yet your core and outer hip muscles might get weaker from lack of engagement. So what? Well, these muscle imbalances often lead to skeletal imbalances and injuries down the line. If you have particularly tight hip flexors, your body will start to create an anterior pull on the pelvis (anterior pelvic tilt). You can identify an anterior pelvic tilt if your belly protrudes slightly in the front while your butt sticks out in the back (what some people refer to as “duck butt”).

Hip tendonitis is inflammation of any of the hip tendons, or thick cords that attach muscles to bone. Similar to strains, hip tendonitis is commonly caused by overuse. And, also like strains, tendonitis frequently affects the same population—athletes who participate in cycling, swimming, running, and other sports that repeatedly stress the hip. High intensity interval training (HIIT) workouts and other activities that involve a high volume of kicking, squatting, and jumping can also lead to tendon inflammation.
Strengthening exercises, beyond general daily activities, are not advised for acute low back pain, but may be an effective way to speed recovery from chronic or subacute low back pain. Maintaining and building muscle strength is particularly important for persons with skeletal irregularities. Health care providers can provide a list of beneficial exercises that will help improve coordination and develop proper posture and muscle balance. Evidence supports short- and long-term benefits of yoga to ease chronic low back pain.
Discography may be used when other diagnostic procedures fail to identify the cause of pain. This procedure involves the injection of a contrast dye into a spinal disc thought to be causing low back pain. The fluid’s pressure in the disc will reproduce the person’s symptoms if the disc is the cause. The dye helps to show the damaged areas on CT scans taken following the injection. Discography may provide useful information in cases where people are considering lumbar surgery or when their pain has not responded to conventional treatments.


